- Embarrassed by your feet?
- Ever wondered what a podiatrist can actually do?
- Wondering if you could benefit from seeing a podiatrist?
Then check out this blog which explains the top 5 conditions podiatrists see and ways to manage the problems yourself!
1. Corns, callus, split heels
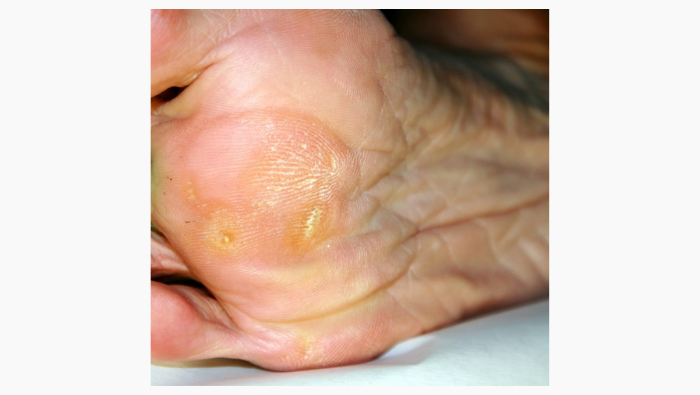
Corns and calluses are areas of hard skin which develop when the skin is exposed to excessive pressure or friction. These areas can often be uncomfortable to walk on and when this happens it is recommended that you visit a HCPC registered podiatrist for further advice and treatment.
Nevertheless, there are a few things you can do to prevent them:
Self management
- Avoid wearing ill-fitting footwear. Shoes that are too tight can cause excessive pressure whilst shoes that are too loose can cause excessive sheering and friction. Slip on shoes are also ones to avoid as they allow your foot to slip and slide, again causing sheering and friction. Slip on shoes can also cause your toes to claw as they desperately try to keep your foot in the shoe. Consequently, this can cause hammer toes which are often associated with the development of corns on the top of the buckled toes.
- Protect any bony areas such as bunions or hammer toes – These deformities are more likely to make footwear harder to fit meaning you are more likely to get excessive pressure or friction.
- Cushion the sole of your feet – whilst good thick soles of shoes are important, as we get older we lose the fatty cushioning pad on the sole of your foot. This exposes the bony prominences which can cause additional pressure on these areas. An insole will offer additional cushioning to these areas.
- Keep the skin hydrated with a urea based emollient such as Gehwol. Dry skin can be more likely to develop into corns and callus. Emollients work best applied twice daily!
- If you start to get rough, dry or hard skin you can use a metal foot file, before bathing or showering. It works best as a prevention, once a week once hard skin has been removed by a podiatrist.
- Corns are a symptom of an underlying problem. Whilst there are products available over the counter such as corn plasters it is best NOT to use these. They often cause far more damage and problems than you think! The best thing is to have them removed by a HCPC registered Podiatrist and address the cause of the problem as best you can.
Cracked heels
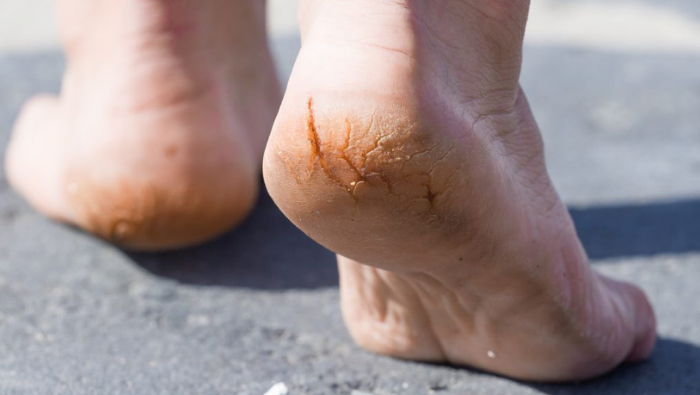
During the warmer weather we are more prone to cracked heels. These can usually be caused by wearing open- backed shoes and the foot rubbing around the edge of the shoe. The fatty pad of your heel also expands sideways in an open-baked shoe which, if the skin is dry, can lead to splitting or cracks within the heels.
To prevent this apply a moisturiser such as flexitol twice a day and use a diamond deb foot file once a week when the skin is dry to reduce the amount of hard skin building up. However if the problem persists you may need to visit a podiatrist who can remove the hard skin and any painful splits and prevent them from getting worse
2. Ingrowing toenails
An ingrowing toenail is where the nail grows into the surrounding skin. This usually affects the big toes although it can affect any toe. The nail can pierce the skin leaving the toe red, swollen and painful. If left it can bleed, discharge pus and eventually become infected.
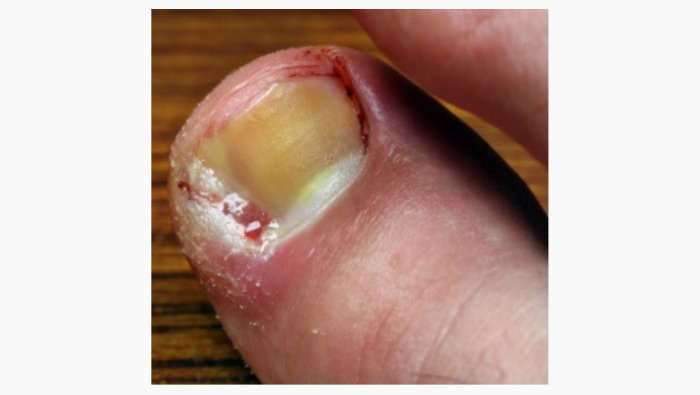
- Cut your nails straight across and not too short, this will prevent the nail from becoming impacted in the surrounding skin as it grows.
- Avoid wearing ill-fitting shoes – shoes which press of the toes adds pressure on the nail. This in turn can promote thickening or changes in the shape of the nail causing it to press into the surrounding skin.
- It’s not just the shoes – socks or tights which are too tight can do exactly the same thing!
- Avoid sweaty feet – sweaty feet softens the skin surrounding the nail which makes it easier for the nail to pierce it. Wearing cotton socks and shoes made from breathable materials will help this
- Avoid walking bare foot and in open-toed shoes where injury can be likely. This along with footwear is the most common cause of ingrowing toenails!
If you think you have an ingrowing toenail contact a HCPC Podiatrist who can manage the symptoms and discuss longer term solutions such as minor nail surgery to correct the problem.
3. Fungal nails
It is believe most of us will get a fungal nail at some point in our lives however it is important to know that not all thickened nails or discoloured nails are in fact fungal nails. Damage, extensive use of false nails or nail polish, medical conditions and deficiencies are just some of the other possible causes of discoloured or thickened nails.
A fungal nail usually causes the following changes (although it is best to have a podiatrist give a confirmed diagnosis before starting any treatment).
- Discolouration
- Thickness
Most fungal nails are caused because of an undiagnosed and untreated athletes foot infection on the skin. This usually looks a bit red or scaly and can be very itchy. Contrary to popular belief it is not only found in between the toes but can be anywhere on feet, particular borders and arch of your feet. Fungus like; warmth, dark and moisture and we are providing all 3 with our feet!
So it is important to
- wash and dry your feet regularly
- don’t wear shoes which may cause your feet to get too sweaty!
- Wearing cotton socks rather than going without socks or wearing nylon will also help
- ensure all the infection of athletes foot is cleared up and you are preventing it from reoccurring before starting any treatment for the fungal nails.
When to see a podiatrist?
There are lots of very expensive treatments on the market which all claim to be the best at treating fungal nails. Before you embark on any of these treatments I would suggest you have the nail tested to confirm the presence of fungus. This is a quick, easy and reliable test which can be done in clinic. Once a diagnosis has been confirmed, treatment plans can be discussed and the best treatment given for your problem. 3
4. Verruca
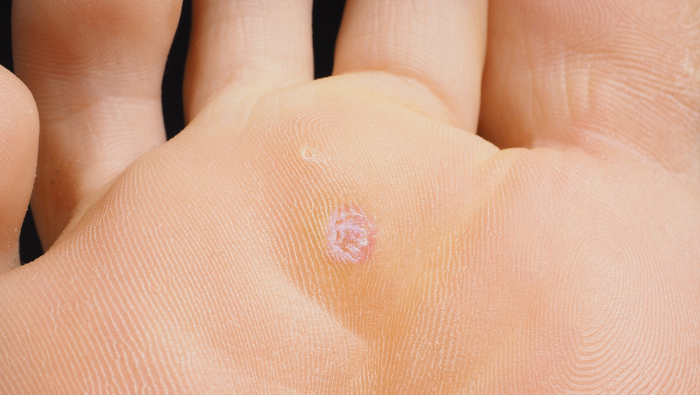
Verruca (or verrucae if there are more than one), is the term given to describe a wart on the foot. It is the same as a wart elsewhere on the body but when it is found on the foot, we use the term verruca. There are about 200 different subtypes of wart but we mainly see 3 on the foot.
Verruca can present as a singular lesion or as multiple lesions often in a mosaic pattern.
How does it get into the skin?
The virus can be found everywhere, but when there is a break in the skin, the virus can enter your body and present as a verruca. Research shows that the virus normally lies dormant for up to 9 months before it develops into the skin lesion you see before you. In most cases they aren’t painful, but if a lot of callus builds up over the top or it is situated on a high-pressure area then they can become painful.
Latest research suggests in most cases the body isn’t aware of the verruca because of where it develops. So, it is not linked with low immunity.
Is it contagious?
Although contagious, you need a break in the surface of the skin to allow the virus to enter your body. This can be non-slip tiles at the swimming pool or even walking barefoot on hard flooring at home can cause minor abrasions to the surface of the skin which allows the virus in. For this reason, the risk of you “catching” them from another member of your family is low. You would first need a break in the surface of the skin as described above, along with skin to skin contact to allow the transfer of the virus.
What Can you do?
- The best thing is to leave it alone, although if its painful, persistant or bothers you and you would like to discuss treatments, speak to a HCPC podiatrist about treatment options.
- Wear flip fops around house and swimming pool
5. Diabetes
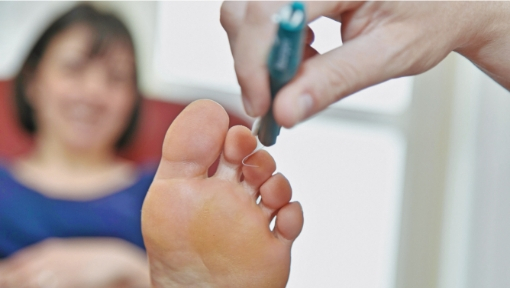
Diabetes may affect your feet in a number of ways and in some cases can lead to serious complications. One of the early changes can be loss of sensation in your feet often starting at the toes. This may be gradual and go unnoticed which is why it is important that you receive an annual foot assessment with a Podiatrist. When the nerves are affected other changes may follow. Your toes may begin to change shape and claw and the bones in your feet can become more susceptible to fractures.
Here is some simple advice for anyone with diabetes
- Always check your feet everyday looking for any colour changes or damage to the skin. If you see anything unusual contact your podiatrist to get it checked.
- Clean and dress any cuts or scratches as diabetes can affect the way you heal and reduce your natural ability to fight infection.
- Avoid walking barefoot as you may have lost some feeling in your feet and it may be possible to unknowingly damage them.
- Always ensure your shoes fit correctly
- Never sit with your feet too close to a fire
- Always check inside your shoes with your hand before putting them on for any added delights that may have fallen in!
- It you have any bony prominences to your feet – check for rubbing and protect them with a silipos pad if required.
- If you have corns and calluses get these removed by a Podiatrist as it can lead to ulceration if left untreated.
- Do not under any circumstances use corn plasters! They burn holes in the skin and can lead to ulcerations!
So don’t be embarrassed we have seen it all! If you would like to discuss any foot problems with a podiatrist, contact us today.


